SYSTEMATIC REVIEW WITH META-ANALYSIS OF OBESITY AS RISK FACTOR OF COVID-19 RELATED MORTALITY
Downloads
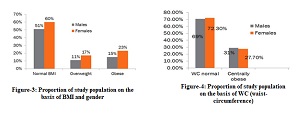
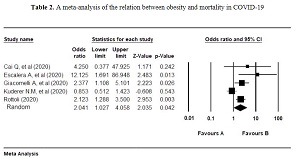
A person with obesity has a high risk of getting a severe complication of COVID-19. This is related to the increasing of chronic illness cases caused by obesity. Obesity itself has been known to take part in the disruption of the human immune system. A person with obesity will be more susceptible to the infection and is suspected to be one of the risk factors that cause death in COVID-19. This study used observational analysis with a systematic review method and continued with Meta-Analysis. This study has been held at the Public Health Department of Faculty of Medicine, Universitas Airlangga, Surabaya, in July 2020. The data sources of this study come from online literature, such as published journals that match our inclusion criteria. The inclusion criteria for this study were journals that study the relation of obesity and mortality in COVID-19 cases, journals with a cross-sectional design, journals that used samples age >18 y.o., and journals that used BMI as the obesity classification. Five journals matched our criteria and were analyzed in this study. Four of 5 journals show that there is a relationship between obesity and mortality of COVID-19. There are 2133 subjects with COVID-19, and 361 of them have obesity. There are 1861 subjects with COVID-19 who are not dead; 1567 of them don't have obesity. An analytic study with a random effect model shows that obesity is the risk factor of mortality in COVID-19 cases (OR = 2.041; 95% CI 1.027-4.058). It also shows that there is a significant relationship between obesity and mortality in COVID-19 cases (p=0.042). Most journals analyzed with a systematic review and meta-analysis in this study show that obesity is the risk factor of mortality in COVID-19 cases.
Li Q, Guan X, Wu P, et al (2020). Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus–Infected Pneumonia. New England Journal of Medicine, 382(13), 1199-1207 DOI: 10.1056/NEJMoa2001316.
WHO (2020). WHO Coronavirus Disease (COVID-19) Dashboard, https://covid19.who.int/
Kementerian RI (2020). Gugus Tugas Percepatan Penanganan COVID-19, https://covid19.go.id/peta-sebaran
Hruby A, Hu FB (2015). The Epidemiology of Obesity: A Big Picture. Pharmaco Economics. 33(7), 673-689. DOI: 10.1007/s40273-014-0243-x.
Finer N, Garnett SP, Bruun JM (2020). COVID-19 and obesity. Clinical Obesity. 10(3), e12365. DOI: https://doi.org/10.1111/cob.12365.
Gao M, Piernas C, Astbury NM, et al (2021). The Lancet Diabetes & Endocrinology. 9(6), 350-359. DOI: 10.1016/S2213-8587(21)00089-9.
Kassir R (2020). Risk of COVID-19 for patients with obesity. Obes Rev. 21(6), e13034. DOI: 10.1111/obr.13034.
Cai Q, Huang D, Ou P, et al (2020). COVID-19 in a designated infectious diseases hospital outside Hubei Province, China. Allergy, 75(7), 1742-1752. DOI: 10.1111/all.14309.
Escalera-Antezana JP, Lizon-Ferrufino NF, Maldonado-Alanoca A, et al (2020). Clinical features of the first cases and a cluster of Coronavirus Disease 2019 (COVID-19) in Bolivia imported from Italy and Spain. Travel Med Infect Dis, 35, 101653. DOI: 10.1016/j.tmaid.2020.101653.
Giacomelli A, Ridolfo AL, Milazzo L, et al (2020). 30-day mortality in patients hospitalized with COVID-19 during the first wave of the Italian epidemic: A prospective cohort study. Pharmacol Res. 158, 104931. DOI: 10.1016/j.phrs.2020.104931.
Rottoli M, Bernante P, Belvedere A, et al (2020). How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients? Results from a single Italian centre. European Journal of Endocrinology. 183(4), 389-397. DOI: 10.1530/eje-20-0541.
Kuderer NM, Choueiri TK, Shah DP, et al (2020). Clinical impact of COVID-19 on patients with cancer (CCC19): a cohort study. The Lancet. 395(10241), 1907-1918. DOI: 10.1016/S0140-6736(20)31187-9.
Dixon AE, Peters U (2018). The effect of obesity on lung function. Expert Rev Respir Med. 12(9), 755-767. DOI: 10.1080/17476348.2018.1506331.
Marazuela M, Giustina A, Puig-Domingo M (2020). Endocrine and metabolic aspects of the COVID-19 pandemic. Reviews in endocrine & metabolic disorders. 21, 495-507. DOI: 10.1007/s11154-020-09569-2.
Mohammad S, Aziz R, Al Mahri S, et al (2021). Obesity and COVID-19: what makes obese host so vulnerable? Immun Ageing. 18(1), 1.
DOI: 10.1186/s12979-020-00212-x.
Sanchis-Gomar F, Lavie CJ, Mehra MR, et al (2020). Obesity and Outcomes in COVID-19: When an Epidemic and Pandemic Collide. Mayo Clinic Proceedings, 95(7), 1445-1453. DOI: 10.1016/j.mayocp.2020.05.006.
Cava E, Neri B, Carbonelli MG, et al (2021). Obesity pandemic during COVID-19 outbreak: Narrative review and future considerations. Clinical nutrition (Edinburgh, Scotland), 40(4), 1637-1643.
DOI: 10.1016/j.clnu.2021.02.038.
Huang Y, Lu Y, Huang Y-M, et al (2020). Obesity in patients with COVID-19: a systematic review and meta-analysis. Metabolism: clinical and experimental, 113, 154378-154378. DOI: 10.1016/j.metabol.2020.154378.
Sattar N, McInnes IB, McMurray JJV (2020). Obesity Is a Risk Factor for Severe COVID-19 Infection. Circulation, 142(1), 4-6. DOI: 10.1161/CIRCULATIONAHA.120.047659.
Popkin BM, Du S, Green WD, et al (2020). Individuals with obesity and COVID-19: A global perspective on the epidemiology and biological relationships. Obesity Reviews. 21(11), e13128.
Copyright (c) 2021 Achmad Ilham Rizwani, Syarif Syamsi Ahyandi, Nanning Naimatuningsih, Endy Novryan Ridwan, Rani Nurvita, Nurun Nujum, Muhammad Hammam Mahrus, Lilik Djuari

This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
- The journal allows the author to hold the copyright of the article without restrictions.
- The journal allows the author(s) to retain publishing rights without restrictions.
- The legal formal aspect of journal publication accessibility refers to Creative Commons Attribution Share-Alike (CC BY-SA).
- The Creative Commons Attribution Share-Alike (CC BY-SA) license allows re-distribution and re-use of a licensed work on the conditions that the creator is appropriately credited and that any derivative work is made available under "the same, similar or a compatible license”. Other than the conditions mentioned above, the editorial board is not responsible for copyright violation.