Association Between Dietary Patterns of Salty Foods, Sweet Drinks, Fruit and Vegetables and The Prevalence of Hypertension in East Java: Multivariate Analysis of Indonesian Basic Health Surveys Data 2018
Downloads
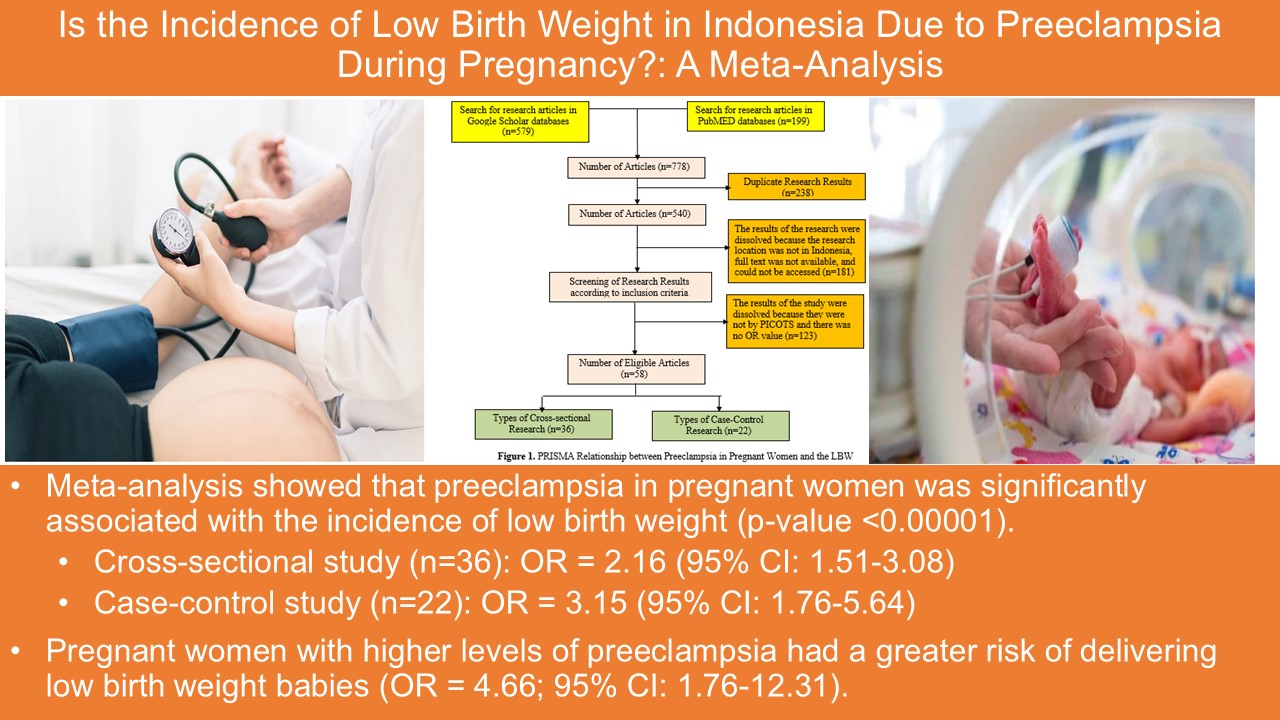
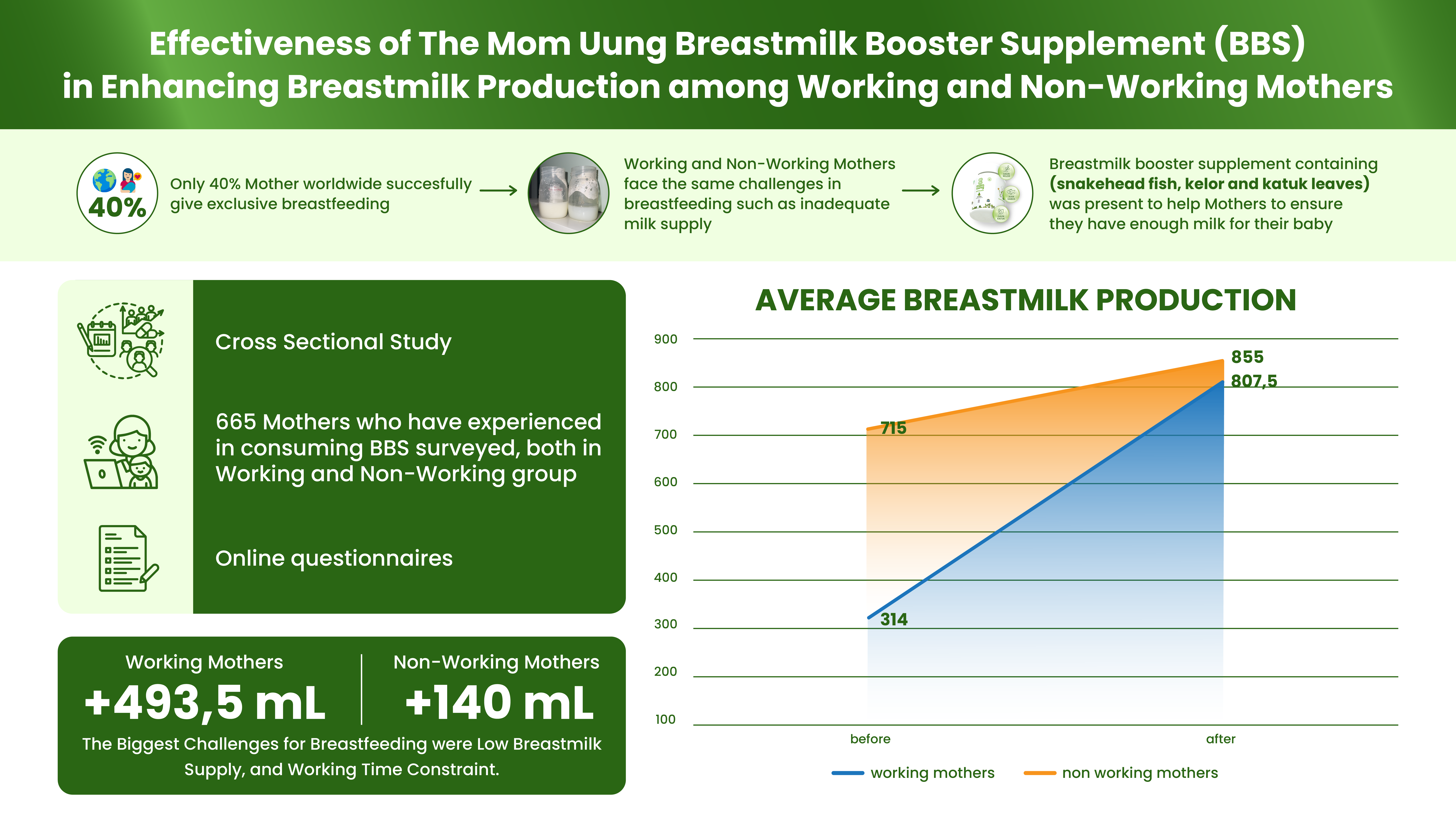
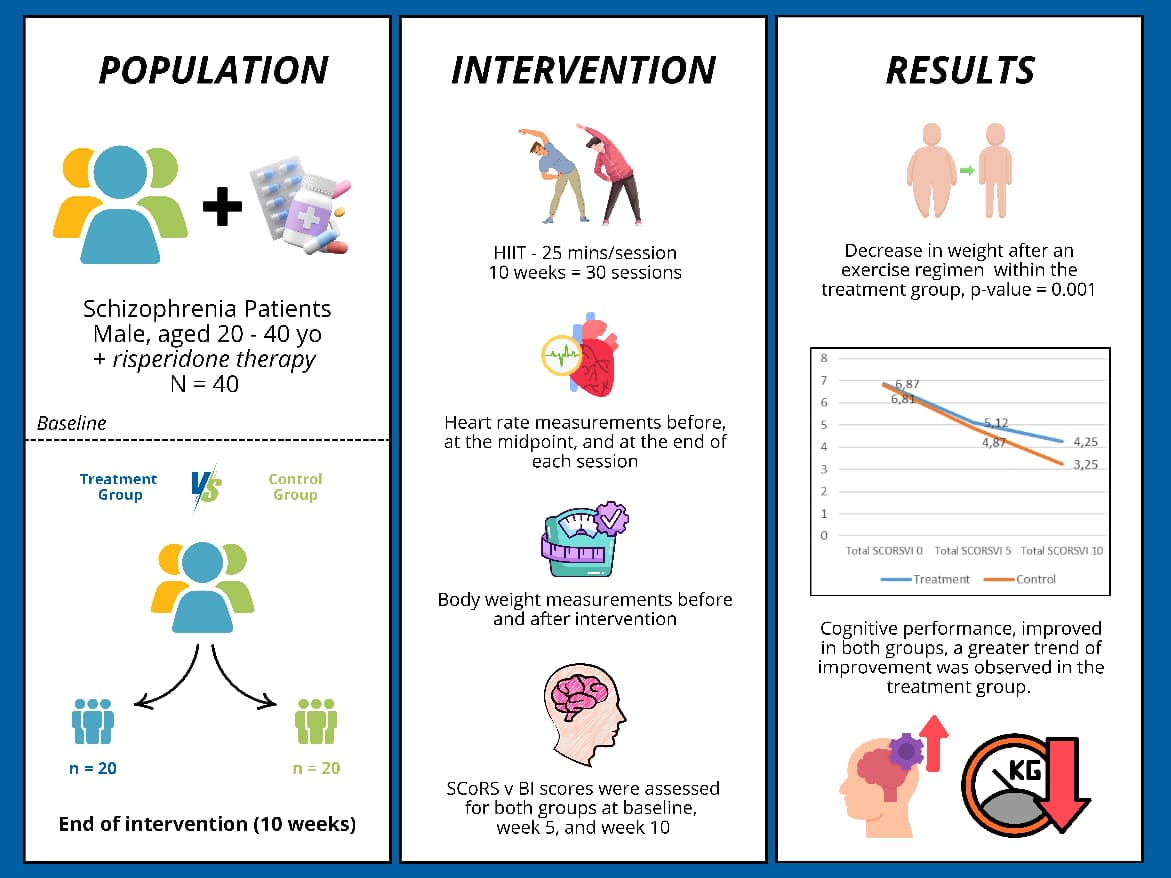
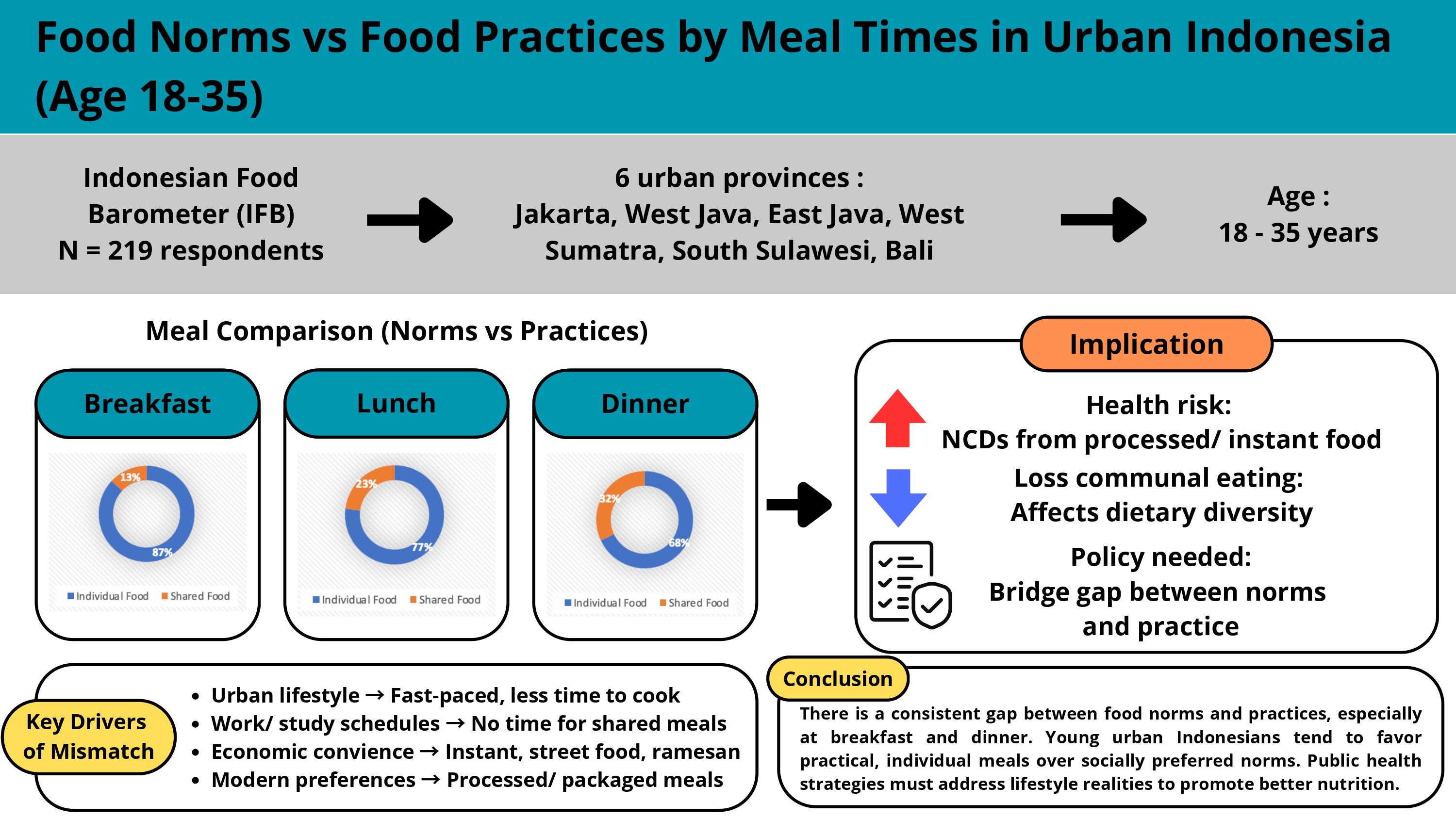
Hypertension remains the main cause of mortality globally, including in Indonesia, with a prevalence rate of 34.1%. Various studies have reported an association between dietary patterns and the prevalence of hypertension. Therefore, further analysis is needed to determine preventive intervention strategies in each region. This study aimed to analyze the effect of dietary patterns on the prevalence of hypertension in East Java Province. The sample is the result of multistage random sampling from the census block of Basic Health Research (Riskesdas) report in the East Java Province collected from 2013 – 2018. The classical assumption test was carried out using the Kolmogorov-Smirnov method, bivariate test using the Pearson method, and multivariate test using the multiple linear regression method. There are three variables tested that have a p-value below the value of α <0.05, including eating salty foods once a day (p=0.021), drinking sweet drinks three times per month (p=0.008), and non-routine of fruits and vegetables consumption (p=0.003). Based on the r-value, the association between predictor variables and prevalence in order from the largest to the smallest of the habit of not consuming fruits and vegetables (r=-0.469), the habit of drinking sugary drinks three times per month (r=-0.425), and salty eating habits one time per day (r=-0.372). Multivariate multiple linear regression analysis showed that daily intake of salty foods (p=0.013) was associated with the prevalence of hypertension.
Adrogué HJ, Madias NE. Sodium and potassium in the pathogenesis of hypertension. N Engl J Med. 2007;356(19):1966–78.
Arima H, Barzi F, Chalmers J. Mortality patterns in hypertension. J Hypertens. 2011;29:S3–7.
Carretero OA, Oparil S. Essential hypertension: part I: definition and aetiology. Circulation. 2000;101(3):329–35.
Cohen L, Curhan G, Forman J. Association of sweetened beverage intake with incident hypertension. J Gen Intern Med. 2012;27(9):1127–34.
Forouzanfar MH, Liu P, Roth GA, Ng M, Biryukov S, Marczak L, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990-2015. Jama. 2017;317(2):165–82.
He FJ, MacGregor GA. How far should salt intake be reduced? Hypertension. 2003;42(6):1093–9.
Kesehatan Kementerian RI. Laporan Provinsi Jawa Timur Riset kesehatan dasar (Riskesdas) 2018. Jakarta Badan Penelit dan Pengemb Kesehat Kementrian Kesehat Republik Indones. 2018;
Kesehatan Kementerian RI. Riset kesehatan dasar (Riskesdas) 2018. Jakarta Badan Penelit dan Pengemb Kesehat Kementrian Kesehat Republik Indones. 2018;
Krishnan A, Garg R, Kahandaliyanage A. Hypertension in the South-East Asia region: an overview. In: Regional health forum. 2013. p. 7–14.
Kwak JH, Jo G, Chung H-K, Shin M-J. Association between sugar-sweetened beverage consumption and incident hypertension in Korean adults: a prospective study. Eur J Nutr. 2019;58(3):1009–17.
Maersk M, Belza A, Stí¸dkilde-Jí¸rgensen H, Ringgaard S, Chabanova E, Thomsen H, et al. Sucrose-sweetened beverages increase fat storage in the liver, muscle, and visceral fat depot: a 6-mo randomized intervention study. Am J Clin Nutr. 2012;95(2):283–9.
Malik VS, Pan A, Willett WC, Hu FB. Sugar-sweetened beverages and weight gain in children and adults: a systematic review and meta-analysis. Am J Clin Nutr. 2013;98(4):1084–102.
RI K. Laporan hasil riset kesehatan dasar (Riskesdas) Indonesia tahun 2018. Jakarta Badan Penelit dan Pengemb Kesehat Kemenkes RI. 2018;5–10.
Schwingshackl L, Schwedhelm C, Hoffmann G, Lampousi A-M, Knüppel S, Iqbal K, et al. Food groups and risk of all-cause mortality: a systematic review and meta-analysis of prospective studies. Am J Clin Nutr. 2017;105(6):1462–73.
Singh S, Shankar R, Singh GP. Prevalence and associated risk factors of hypertension: a cross-sectional study in urban Varanasi. Int J Hypertens. 2017;2017.
Suh I. PL 01-2 blood pressure and cardiovascular disease mortality in the Asia Pacific Region. J Hypertens. 2016;34:e11.
Turana Y, Widyantoro B, Situmorang TD, Delliana J, Roesli RMA, Danny SS, et al. May Measurement Month 2018: an analysis of blood pressure screening results from Indonesia. Eur Hear J Suppl. 2020;22(Supplement_H):H66–9.
World Health Organization. A global brief on hypertension: silent killer, global public health crisis: World Health Day 2013. World Health Organization; 2013.

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
- MEDIA GIZI INDONESIA Journal is the copyright owner of all materials published on this website.
- The formal legal provisions for access to digital articles of this electronic journal are subject to the terms of the Creative Commons Attribution-NonCommercial-ShareAlike license (CC BY-NC-SA 4.0), which means that MEDIA GIZI INDONESIA Journal and readers reserve the right to save, transmit media / format, manage in database, maintain, and publish articles as long as it continues to include the name of the Author.
- Printed and published print and electronic manuscripts are open access for educational, research and library purposes. In addition to these objectives, the editorial board shall not be liable for violations of copyright law.


2.png)