Faktor Risiko Dropout Kontrasepsi Suntik Progesteron
Downloads
Introduction: Prevention effort of progestogen-only prevalence rate injectable discontinuation has not got the national target and it always increases. The prevalence rate is one of causes Total Fertility Rate (TFR) increasing. The study analyzed the risk factors associated with the progestogen-only injectable discontinuation case.
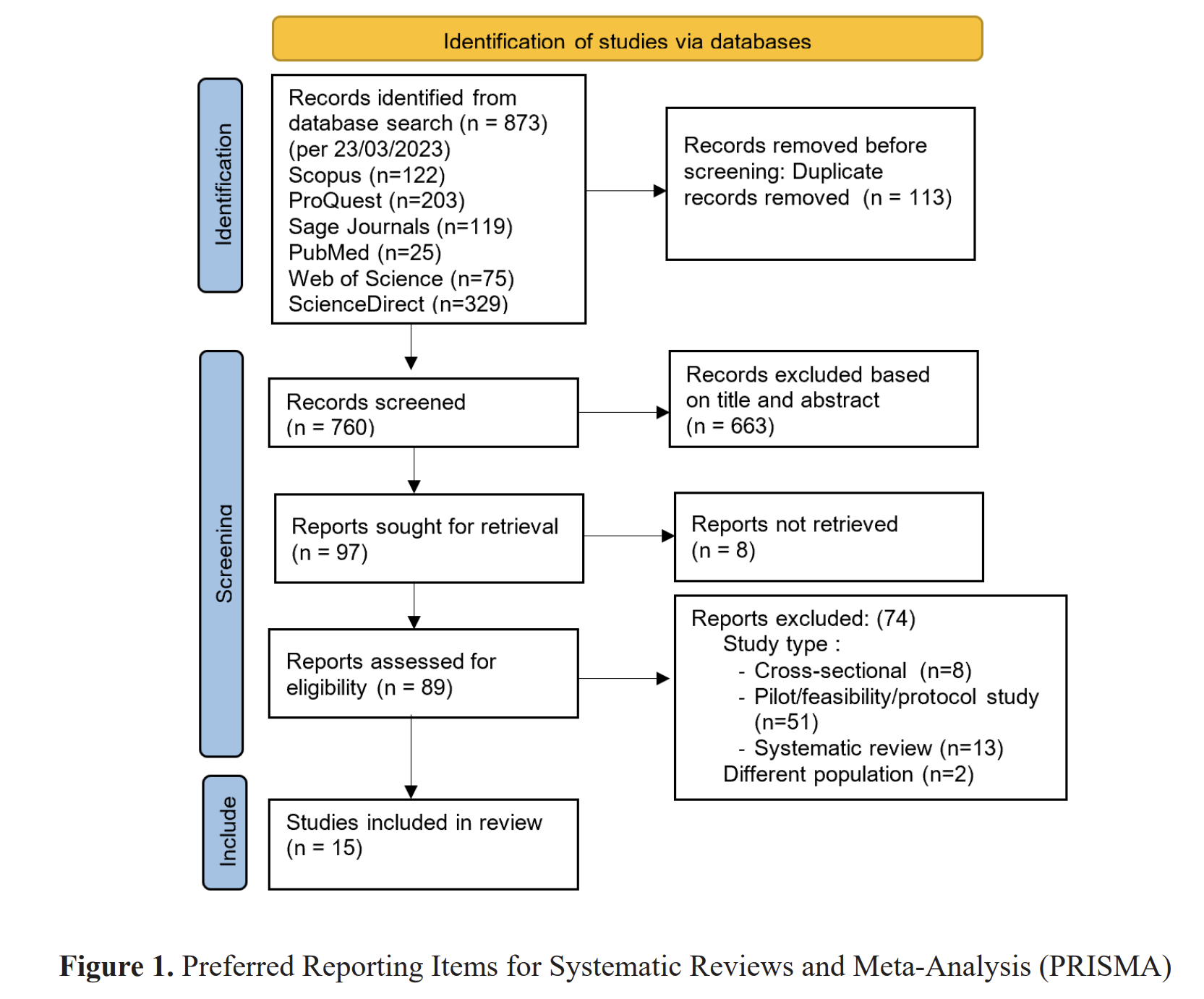
Methods: This study used analytic observational with cross sectional design which was carried out in Puskesmas Mojo Surabaya on March – April 2019. Population are 646 discontinuation acceptors and 5,751 non discontinuation acceptors of progestogen-only injectable. The inclusion criteria were acceptors of progestogen-only injectable discontinuation case, have a husband, not yet menopause. The exclusion criteria were acceptor of progestogen-only injectable discontinuation who used other contraception. Total samples are 44 samples obtained by with consecutive sampling. Independent variables were desire pregnancy, myths, weight change, spotting, amenorrhea, husband support. Dependent variable was the progestogen-only injectable discontinuation case. The data are collected by questionnaire, analyzed by chi-square test with α < 0.005 and multivariate analysis with independent variable p<0.25
Results: The factor which correlated with the progestogen-only injectable discontinuation was husband support (p=0.012). The factors which not correlated with the case are desire pregnancy (p=1.000), myths (p=0.138), weight change (p=0.378), spotting (p=0.164), amenorrhea (p=0.192). The dominant factor was husband support (Odds Ratio = 26.571; 95%Cl = 2.497–282.736).
Conclusion: The dominant factor in this study is husband support.
Riskesdas (Riset Kesehatan Dasar). Riset Kesehatan Dasar. Jakarta; 2013.
Dinas Kesehatan Surabaya. Jumlah Dropout Peserta KB Suntik 3 Bulan di Puskesmas Kota Surabaya Tahun 2013-2017. Surabaya; 2018.
BKKBN. Laporan Akuntabilitas Kinerja Instansi Pemerintah 2017. Priohutomo S, editor. Jakarta: Badan Kependudukan dan Keluarga Berencana Nasional; 2017.
Population Reference Bureau. World Population Data Sheet. 2015 World Population Data Sheet. 2015. 23 p.
BKKBN. Laporan Akuntabilitas Kinerja Instansi Pemerintah 2015. 2015. 95 p.
Affandi B. Buku Panduan Praktis Pelayanan Kontrasepsi. Jakarta: Bina Pustaka Sarwono Prawirohardjo; 2014.
Gichuhi JW, Referral M. The Effect Of Depot Medroxyprogesterone Acetate Contraceptive On Body Weight And Blood Pressure In Indigenous Kenyan Women. Eur Int J Sci Techn ology. 2014;3(6):37–46.
Njoku CO, Emechebe CI, Iklaki CU, Njoku AN, Ukaga JT. Progestogen-Only Injectable Contraceptives: The Profile of the Acceptors, Side Effects and Discontinuation in a Low Resource Setting, Nigeria. Open J Obstet Gynecol. 2016;06(04):189–95.
Shafaie FS, Homayounfar N, Malaquti J, Amani F. Compare of continuation rate and reasons for discontinuation of DMPA contraceptive among Iranian women referred to Tabriz and Ardebil health centers. Int J Women's Heal Reprod Sci. 2014;2(4):240–4.
Veisi F, Zangeneh M. Comparison of Two Different Injectable Contraceptive Methods: Depo-medroxy Progesterone Acetate (DMPA) and Cyclofem. J Fam Reprod Heal. 2013;7(3):109–13.
Maharjan M, Tongkumchum P, Kakchapati S. Social determinants of discontinuation of depo-provera among married women in Nepal. Edorium J Public Heal. 2016;6(August):1–3.
Khan ME, Dixit A, Ahmad J, Pillai G. Introduction Of DMPA in Public Health Facilities of Uttar Pradesh and Rajasthan: An Evaluation. New Delhi, India: The Population Council; 2015.
Castle S, Askew I, Harcourt J, Dasgupta A, Longfield K. Contraceptive Discontinuation: Reasons, Challenges, and Solutions. Family Planning 2020 Population Council. London: Family Planning 2020, Population Council; 2015. 6–10 p.
Outlook. Countering Myths and Misperceptions about Contraceptives. June 2015. Outlook on Reproductive Health. USA: Path; 2015.
Hofmeyr GJ, Singata-Madliki M, Lawrie TA, Bergel E, Temmerman M. Effects of the copper intrauterine device versus injectable progestin contraception on pregnancy rates and method discontinuation among women attending termination of pregnancy services in South Africa: A pragmatic randomized controlled trial. Reprod Health. 2016;13(1):1–8.
Mufdlilah M, Aryekti K. Factors Causing Contraceptive Acceptors Drop Out. Kesmas Natl Public Heal J. 2018;12(4):202.
Ali MM, Cleland J, Shah IH. Causes and consequences of contraceptive discontinuation. World Health Organization. Egypt: World Health Organization; 2012.
Santelli J, Lindberg LD, Orr MG, Finer LB, Speizer I. Toward A Multimedimensional Measure of Pregnancy Intentionts: Evidence from The United States. Stud Fam Plann. 2009;40(87–100).
Lacovou M, Tavares LP. Yearning, Learning, And Conceding: Reasons Men And Women Change Their Childbearing Intentions. Popul Dev Rev. 2011;37(89–123).
Joyce T, Kaestner R, Korenman S. The Stability Of Pregnancy Intentions And Pregnancy-Related Maternal Behaviors. Matern Child Heal J. 2000;4(171–8).
Sheffler KM, Greil AL, Mitchell KS, McQuillan J. Variation In Pregnancy Intendedness Across U.S. Women's Pregnancies. Matern Child Heal J. 2015;19(932–8).
Luker KC. A Reminder That Human Behavior Frequently Refuses To Conform To Models Created By Researchers. Farm Plann Perspect. 1999;31(248–9).
Morgan SP, Rackin H. The Correspondence Between Fertility Intentions And Behavior In The United States. Popul Dev Rev. 2010;36(91–118).
Schoen R, Astone NM, Kim YJ, Nathanson CA, Fields JM. Do Fertility Intentions Affect Fertility Behavior? J Marriage Farm. 1999;61(790–9).
Messer LC, Dole N, Kaufman JS, Savitz DA. Pregnancy Intendedness, Maternal Psychosocial Factors and Preterm Birth. Matern Child Heal J. 2005;9(403–12).
Klerma LV. The Intendedness of Pregnancy: A Concept in Transition. Matern Child Heal J. 2000;20(155–62).
Cha S, Chapman DA, Wan W, Burton CW, Macho SW. Discordant Pregnancy Intentions In Couples And Rapid Repeat Pregnancy. Am J Obs Gynecol. 2016;214(494):1–12.
Borrero S, Nikolajski C, Steinberg JR, Freedman L, Akers AY, Ibrahim S. ‘"It just happens”': a qualitative study exploring low-income women's perspectives on pregnancy intention and planning. Contraception. 2015;91(150–6).
Higgins JA, Popkin RA, Santelli JS. Pregnancy Ambivalence And Contraceptive Use Among Young Adults In The United States. Perspect Sex Reprod Heal. 2012;44(2):36–43.
Kagesten A, Bajos N, Bohet A, Moreau C. Male Experiences Of Unintended Pregnancy: Characteristics And Prevalence. Hum Reprod. 2015;30(186–96).
Mumford SL, Ph D, Sapra KJ, Ph D, King RB, Ph D, et al. Pregnancy intentions ” a complex construct and call for new measures. Fertil Steril. 2016;(34).
Sarah Castle. Women's Social Networks, Family Planning Use and Unmet Need: Formative Research Findings from Terikunda Jékulu. United State: USAID; 2011.
Gueye A, Org A. Belief in Family Planning Myths at the Individual And Community Levels and Modern Contraceptive Use in Urban Africa HHS Public Access. Int Perspect Sex Reprod Heal. 2015;41(4):191–9.
Diamond-Smith N., Campbell M., S. Madan. Misinformation and Fear of Side Effects of Family Plan- ning. Cult Heal Sex. 2012;14(4):421–33.
Ningsih Y. Hubungan Intensitas Nyeri Akut dengan Tekanan Darah Pada Pasien di Rumah Sakit Umum Daerah Temanggung. J Phys Educ Heal Sport. 2016;3(2):135–43.
McArdle W, Katch F, Katch V. Exercise Physiology: Nutrition, Energy, and Human Performance. 2010.
Beksinska ME, Smit JA, Kleinschmidt I, Milford C, Farley TMM. Prospective study of weight change in new adolescent users of DMPA, NET-EN, COCs, nonusers and discontinuers of hormonal contraception. Contraception. 2010;81(1):30–4.
Medforth J. Kebidanan Oxford: dari Bidan untuk Bidan. Praptiani W, editor. Jakarta: EGC; 2011. 524–526 p.
Lopez LM, Edelman A, Chen-Mok M, Trussell J, Helmerhorst frans M. Progestin-only contraceptives : Effects on Weight (Review) Summary of Findings for The Main Comparison. Group CFR, editor. The Cochrane Collaboration. USA: John Wiley & Sons, Ltd.; 2013.
Qonitun U. Hubungan Antara Efek Samping Kontrasepsi Dmpa Dengan Kejadian Drop Out Pada Pasangan Usia Subur (Pus) Di Desa Mandirejo Kecamatan Merakurak Kabupaten Tuban. J Midpro. 2017;9(2):30–4.
Mirah DA. Perbedaan Perubahan Berat Badan Pengguna Kontrasepsi Suntik DMPA dan Kombinasi (DMPA dan Estrogen) Berdasarkan Lama Penggunaan di BPM Farida Hajri Surabaya. Universitas Airlangga; 2017.
Zigler RE, McNicholas C. Unscheduled vaginal bleeding with progestin-only contraceptive use. Am J Obstet Gynecol. 2017;216(5):443–50.
Liu J, Shen J, Diamond-Smith N. Predictors of DMPA-SC continuation among urban Nigerian women: the influence of counseling quality and side effects. Contraception. 2018;
Raidoo S, Kaneshiro B. Unscheduled Bleeding on Hormonal Contraceptives: Pathophysiology, Evaluation, and Management Options. Curr Obstet Gynecol Rep. 2017;6(2):118–25.
Tolley EE, Mckenna K, Mackenzie C, Ngabo F, Munyambanza E. Preferences for A Potential Longer-Acting Injectable Contraceptive: Perspectives From Women, Providers, and Policy Makers in Kenya and Rwanda. Glob Heal Sci Pract. 2014;2(2):182–94.
Prasetyo SE. Analisis Faktor yang Berhubungan dengan Kejadian Drop Out Akseptor KB Kecamatan GunungPati Kota Semarang. Vol. April 2015, Jurnal Ilmu Kesehatan Masyarakat Fakultas Ilmu Keolahragaan Universitas Negeri Semarang. Universitas Negeri Semarang; 2015.
MacLachlan E, Atuyambe LM, Millogo T, Guiella G, Yaro S, Kasasa S, et al. Continuation of subcutaneous or intramuscular injectable contraception when administered by facility-based and community health workers: findings from a prospective cohort study in Burkina Faso and Uganda. Contraception. 2018;98(5):423–9.
Cover J, Namagembe A, Tumusiime J, Nsangi D, Lim J, Nakiganda-Busiku D. Continuation of injectable contraception when self-injected vs. administered by a facility-based health worker: a nonrandomized, prospective cohort study in Uganda. Contraception. 2018;98(5):383–8.
Chirenje ZM, Dhibi N, Handsfield HH, Gonese E, Tippett Barr B, Gwanzura L, et al. The Etiology of Vaginal Discharge Syndrome in Zimbabwe: Results from the Zimbabwe STI Etiology Study. Sex Transm Dis Assoc. 2018;45(6):422–8.
Yuliani NA. Faktor-Faktor yang Berhubungan dengan Keikutsertaan Wanita Pasangan Usia Subur (PUS) dalam Menggunakan Kontrasepsi Intra uterine Device (IUD) di Wilayah Kerja Puskesmas Mojo Surabaya. Universitas Airlangga; 2018.
Mufdlilah, Aryekti K. Dukungan suami terhadap kejadian Drop Out Akseptor Keluarga Berencana (KB) di desa dan kota di Daerah Istimewa Yogyakarta. Musawa. 2016;15(1):103–13.
Copyright (c) 2019 Nur Laila, Budiono Budiono, Sunarsih Sunarsih, Aditiawarman Aditiawarman

This work is licensed under a Creative Commons Attribution 4.0 International License.
1. The journal allows the author to hold the copyright of the article without restrictions.
2. The journal allows the author(s) to retain publishing rights without restrictions.
3. The legal formal aspect of journal publication accessibility refers to Creative Commons Attribution (CC BY).